What is Pulmonary Hypertension?
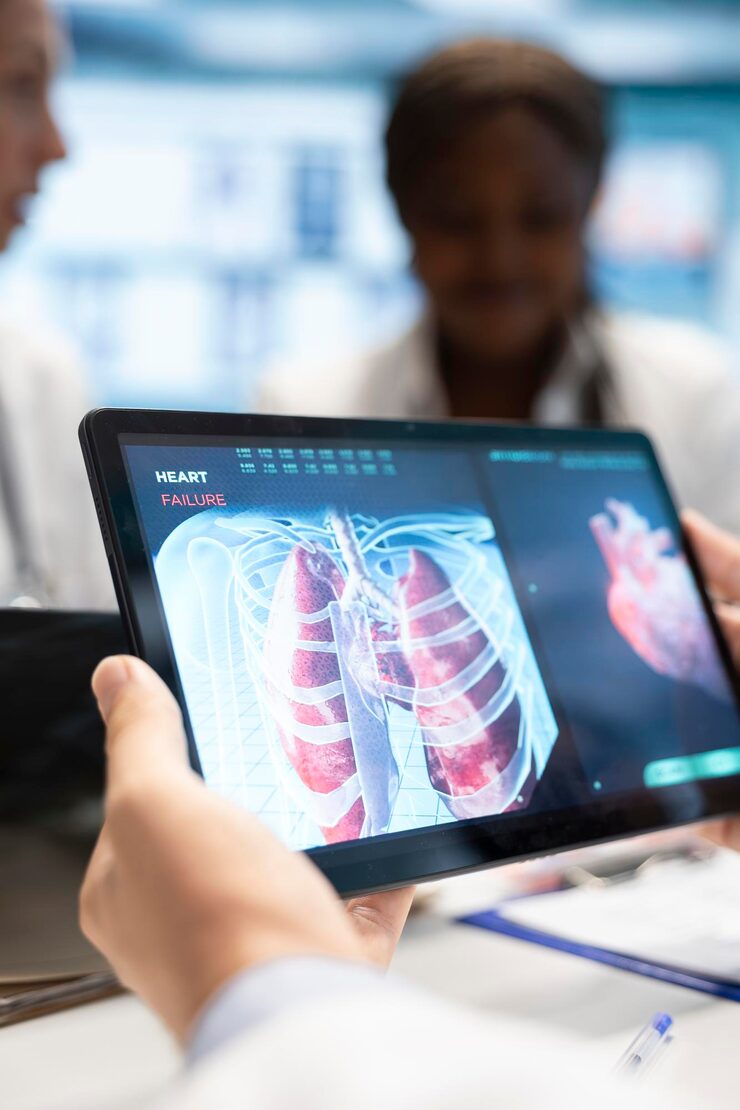
Pulmonary Hypertension occurs when the small arteries in your lungs become narrowed, blocked, or destroyed. This increases the resistance to blood flow, which in turn raises the pressure within the pulmonary arteries. As the pressure builds, the heart’s lower right chamber (right ventricle) must work harder to pump blood through the lungs. Over time, this extra effort causes the heart muscle to weaken and can eventually lead to heart failure.
Pulmonary Hypertension is generally classified into five groups:
- Group 1 (PAH): Pulmonary arterial hypertension caused by genetics, certain drugs, or connective tissue diseases.
- Group 2: PH caused by left-sided heart disease, such as mitral valve problems or long-term high blood pressure.
- Group 3: PH resulting from lung diseases like COPD, pulmonary fibrosis, or sleep apnea.
- Group 4: PH caused by chronic blood clots in the lungs (CTEPH).
- Group 5: PH triggered by other health conditions like blood disorders, sarcoidosis, or metabolic disorders.
At Bio Research Partner, we evaluate PH as a multifaceted condition, addressing the underlying vascular damage while optimizing the systemic environment for cardiovascular resilience.
Causes and Risk Factors
The development of high pressure in the pulmonary circuit is often driven by a combination of vascular changes and external stressors that impair the blood vessels’ ability to dilate.
Risk Factors Include:
- Family History: Genetic predispositions that affect how pulmonary blood vessels grow and react.
- Pre-existing Lung Conditions: Chronic hypoxia (low oxygen) from COPD or sleep apnea that causes vessels to constrict.
- Autoimmune Disorders: Conditions like scleroderma or lupus that cause inflammation in the vascular lining.
- Chronic Liver Disease: Portal hypertension that can lead to increased pressure in the lung circuit.
- Congenital Heart Defects: Structural issues present from birth that alter blood flow patterns.
- Hormonal and Metabolic Fluctuations: Imbalances in nitric oxide production and endothelin levels that regulate vascular tone.
Our approach integrates cardiovascular assessment with metabolic screening to identify the specific drivers of your vascular resistance.